- April 25, 2024
-
-
Loading

Loading
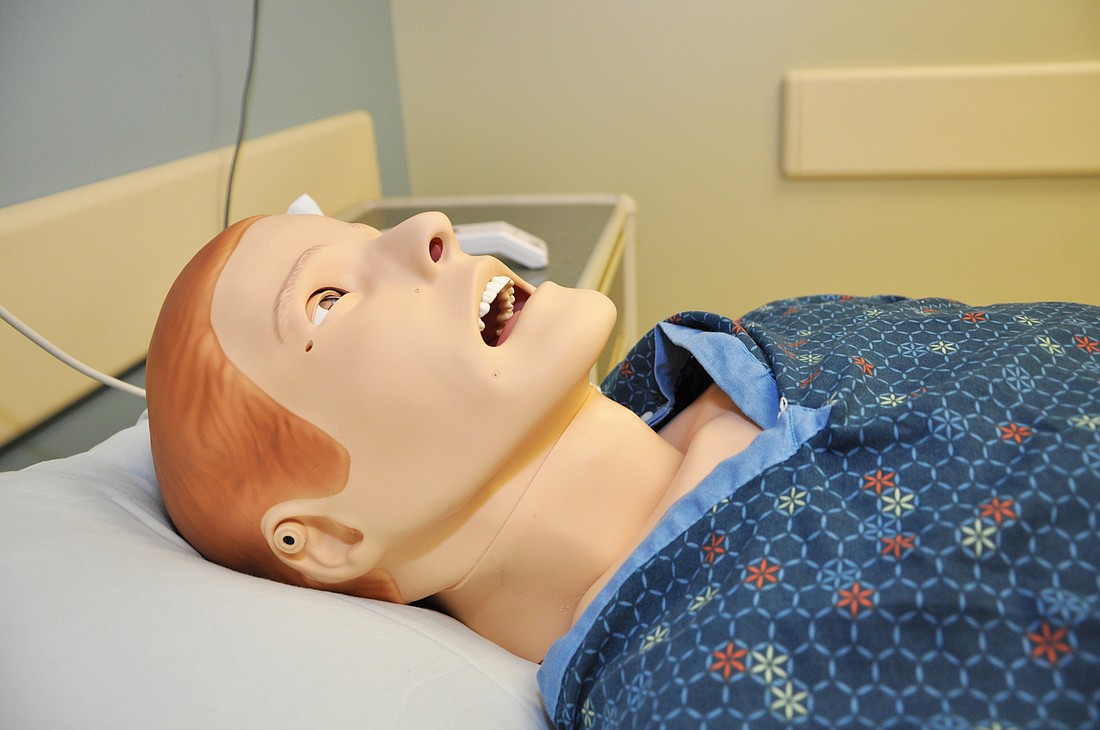
Winter Park Memorial Hospital’s new patient breathes, blinks, talks and has a pulse, but it isn’t human. It’s Sam Winter — the new high-tech mannequin at Winter Park Memorial Hospital used to train nurses and doctors.
Hospital staff had the chance to meet Sam for the first time at an open house event in early October, catching a glimpse of the high-tech patient that can mimic a broad range of symptoms and situations, from heart attacks to child birth.
Sam Winter — a human patient simulator created by Laerdal as the Laerdal SimMan 3G — works through a computer system to mimic human bodily functions. That includes breathing, bleeding, sweating, blinking and talking — done through a microphone system by a training specialist in a separate room. The mannequin also can be changed from male to female simply by switching some of the parts.
Medical staff in training can use the mannequin to check a pulse, give an IV, perform CPR, check for compromised lungs by listening to the breathing and deliver a baby through an automated birthing system — even allowing trainees to go through a variety of birthing scenarios by repositioning the baby inside the mannequin.
“It’s basically a high-fidelity, physiological model that controls almost every human function that you would see in a body,” said Patrick Connors, executive director of simulation at Florida Hospital. “It bleeds, it breathes, it can sweat; it can have discharge from the nose, the eyes, the ears, the mouth; it has very realistic teeth and a jaw, where you can do intubations by putting a tube down the throat. It’s got eyes that blink and eyes that dilate when you put light on them — it’s really cool.”
Trainees can even push “drugs” into the mannequin, Connors said.
“You scan the barcode on the side of the vial — it’s all just distilled water, a clear liquid like all the drugs that you see,” Connors said. “The provider would scan those, and then the computer would know that you’re giving the right medication and the physiological model of the mannequin would react to that. If you push the drugs too fast or too slow or the wrong type, there’s consequences for that.”
The mannequin — named “Sam” because it’s a gender-neutral name and “Winter” after Winter Park — was purchased for about $100,000 for Winter Park Memorial in response to the investment the hospital made in establishing a simulation lab on site, Connors said. Every bit of square footage in a hospital is valuable, and Winter Park Memorial Hospital deserves to have the best technology in place, he said.
“We’ve been on a journey to improve the learning culture across all the Florida Hospitals in Central Florida, and one of the ways to do that is build simulation labs or simulation centers — they’re all different based on the space that you have at each physical location,” Connors said. “They all contain a space where you can go to a safe learning environment away from the patient setting and get practice skills and learn through repetition, observation and debriefing to really get better, reduce risk and increase patient safety.”
“We opened up the sim lab (in Winter Park) probably in 2017,” he said. “I had a lesser-capable mannequin placed there, and then based on the feedback from the staff at Winter Park and the clinical educators, the leaders and what they wanted to do, it became pretty apparent to me that we needed to put a really high-end model over there — that’s the SimMan 3G.”
Connors — who has worked in the simulation field for more than 30 years and served as a U.S. Army colonel training soldiers — knows well the benefits of practicing with a piece of equipment and perfecting techniques. It’s one thing to read about a condition in a book, but it’s another to actually treat it and be in a hospital environment with real doctors, nurses, patients and their families, Connors said. That’s one of the reasons why some training sessions with Sam include role players who might serve as the mannequin’s spouse, daughter or son — it creates a richer learning environment that’s more realistic, Connors said.
“If you’re going to fail, fail early and fail often and do it in a safe place, and then you come out of there with more competence and more confidence in your skills,” Connors said. “You’ve got the education, you’re licensed and you’ve got the degree, but now, it’s time to practice. You know the hard skills, but when you add the complexity of the hospital environment and the complexity and emotion that you have with patients’ interaction with family members, it’s imperative that you practice that before you go onto the floor.
“The more competent you are, the more confident you become,” he said. “It’s a cycle, and it spirals upward.”
Innovation is on the rise in the medical field — and Sam Winter is just a glimpse of how far the technology has come, Connors said. Florida Hospital currently has access to about 77 mannequins — an entire family of “patients” ranging from adults to children to newborns, and it’s all to prepare medical professionals to do their jobs to the best of their ability.
“The technology has gotten better and better, but we’re now moving into not just mannequin-based but augmented reality, where you can look at something through special glasses and then you can see certain wounds or certain things on a mannequin or human,” Connors said. “It’s really changing the learning culture. At Florida Hospital, we’ve come a really long way — we’ve gone from no sim labs to eight different sim labs across the Central Florida footprint. … We’re really moving medical training and medical education to the 21st century like a lot of other industries — like the space industry, nuclear industry, defense industry, etc. I’d say that the health care industry has lagged behind, and now we’re playing rapid catch-up. We realize we have to change the way we embrace technology.
“They’re doing things in that sim lab that we didn’t ever imagine,” Connors said.